The information in this article is critical for expectant parents to provide intel about the diagnosis of prenatal onset hydrocephalus. My intention in this article is simple- to inform readers and parents about precautionary measures to be taken during the time of pregnancy or gestation period. Before we move on, I would like you to introduce you to the subject
What Is Hydrocephalus?
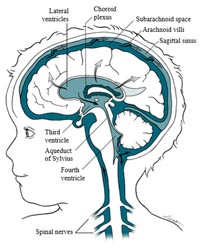
Hydrocephalus is an abnormal accumulation of cerebrospinal fluid (CSF) within cavities called ventricles inside the brain. CSF is produced in the choroid plexus, which is a collection of tissue that rests within the ventricles. CSF surrounds the brain and spinal cord, acting as a protective cushion against injury. It carries nutrients and proteins to the brain while carrying waste products away from surrounding brain tissue.
Under normal conditions, there is a balance between the amount of CSF that is produced and the rate at which it is absorbed. Hydrocephalus is caused most often by an obstruction to the flow pattern of the CSF, but may also result from a failure of CSF to be absorbed into the bloodstream. Because CSF is produced continuously, when an interference with absorption or flow of spinal fluid occurs, CSF will begin to accumulate, causing the ventricles to enlarge and pressure to increase inside the head. When the blockage occurs within the ventricular system, it is called noncommunicating hydrocephalus. If the blockage occurs in the subarachnoid space (outside the ventricles), it is called communicating hydrocephalus, meaning that the ventricles remain open and communicate with each other and the subarachnoid spaces, but CSF can’t be fully absorbed into the bloodstream.
How Is Hydrocephalus Treated?
Shunting is the most common treatment for hydrocephalus. A shunt system, flexible tubing with a one-way valve—is surgically placed in the ventricle to detour excess cerebrospinal fluid from the points of accumulation into another region of the body. In most cases, shunting successfully controls hydrocephalus, but, unlike surgical procedures that can cure a disease, the placement of a shunt does not cure hydrocephalus. Except in rare cases, hydrocephalus is a lifelong condition.
The parts of a shunt are named according to where they are placed in the body. The portion of the tube that is inserted into the ventricles is called the ventricular catheter. If the tube is placed into the peritoneal cavity (the abdomen), it is called a peritoneal catheter. If the tube is placed into the first chamber of the heart (the atrium), it is called the atrial catheter. A valve placed underneath the skin of the scalp opens and closes to control the CSF flow rate based on the pressure within the system and to prevent backward flow of spinal fluid or blood toward the ventricles. Depending on the particular nature of your child’s hydrocephalus, the neurosurgeon will select a valve pressure or flow rate to accommodate your child’s needs.
What Causes Hydrocephalus?
Hydrocephalus is caused by a variety of medical problems including birth defects, in utero infections and malformations within the brain. If hydrocephalus is present before or at birth, it is called congenital hydrocephalus. Many cases of congenital hydrocephalus are thought to be caused by a complex interaction of genetic and environmental factors.
- Aqueductal stenosis, the most common cause of congenital hydrocephalus, is obstruction of the cerebral aqueduct, the long, narrow passageway between the third and fourth ventricles. It may result from narrowing or blockage of the aqueduct by a web or band of tissue, or may be caused by infection, hemorrhage or a tumor.
- Myelomeningocele(or spina bifida), meaning “open spine,” is a neural tube defect (NTD) that occurs during the first trimester of pregnancy, when the fetus is first developing. It is a birth defect that leads to incomplete closure of the tissues and bone over the lower spine, and can affect the development of the central nervous system (CNS). The cause is unknown. The majority of infants with myelomeningocele also have hydro cephalus from a malformation at the top of the neural tube.
- The Chiari II malformation is a downward displacement of the cerebellum and brain stem through the opening at the base of the skull. This malformation blocks the flow of the CSF out of the fourth ventricle, producing hydrocephalus. Chiari II, which is often associated with myelomeningocele, can also affect the shape of other areas of the brain.
- Tumors in children most commonly occur in the back of the brain (the posterior fossa). As a tumor grows, it may fill or compress the fourth ventricle, blocking the flow of spinal fluid and causing hydrocephalus. Tumors also distort the aqueduct and may cause obstruction of the aqueduct or outflow of spinal fluid from the third to fourth ventricle. Tumors anywhere in the ventricles can block CSF circulation and lead to hydro cephalus. Some tumors form from the choroid plexus in the ventricles, causing hydrocephalus by an overproduction of CSF.
- Arachnoid cysts are membranes filled with CSF that can occur anywhere CSF circulates. Some cysts are self contained, while others may be connected by a passageway to the ventricles or subarachnoid space. They block or slow CSF circulation and, if they occur in the pineal region and compress the aqueduct, can cause hydrocephalus.
- Dandy Walker syndrome is a complex change in the structure of the cerebellum that occurs when the midline structures of the cerebellum fail to develop and the fourth ventricle is enlarged. It can be associated with abnormal development of other parts of the brain. It is important to understand that hydrocephalus is a medical condition, not a disease. It is caused by a variety of medical problems and is considered a lifelong condition. Parents must not blame themselves for their child’s hydrocephalus. The circumstances contributing to a child’s hydrocephalus are beyond the parents’ control.
How Is Hydrocephalus Diagnosed in Utero?
Nowadays, it is common practice for pregnant women to have ultrasounds performed at some point in their pregnancy. During this screening, the technician may detect enlarged ventricles, indicating the possible presence of hydrocephalus.
Diagnostic ultrasonography is the most commonly used method for examining pregnant women and tracking fetal development because it allows real-time examination of the fetus while avoiding radiation exposure. Because ultrasonography is sensitive to the interfaces between tissue and water, the size and shape of fetal ventricles can be easily seen. The development of high resolution, real-time ultrasonography has made it possible to examine the cerebral ventricles and the spine, and has led to a greater understanding of the development of the central nervous system—which in turn has enabled in utero detection of conditions like hydrocephalus.
The fetal skull can be discerned via sonography at eight weeks, at which time the intracranial space is occupied by fluid filled cerebral vesicles that will later become the lateral ventricles. By 15 weeks, the lateral ventricles can be detected, and are filled with the choroid plexus. At 20 weeks, the lateral ventricles are still filled by the choroid plexus, but now occupy a smaller portion of the intracranial space. The third ventricle, thalamus and temporal horns also can be recognized at this stage, as can the aqueduct of Sylvius, the brain stem and the basilar cisterns. After 24 weeks, the ventricles usually become progressively smaller, eventually becoming slit like. Other than increased cortical convolutions, the brain undergoes little structural change after 24 weeks.
Hydrocephalus can be detected as early as the latter part of the first trimester. Diagnosis has been made as early as 13 weeks. Around 20 to 24 weeks, abnormal dilation of ventricles is more clearly detectable. The measurement most frequently used for detecting ventricular size is the ratio of lateral ventricle width to cerebral hemisphere width (LVH/HW). This ratio, which normally decreases with gestational age, offers a guidepost for tracking the development of enlarged ventricles.
In certain special cases, magnetic resonance (MR) imaging may be done, especially when normal fluid planes are too obscured for ultrasonography. However, because MR imaging requires a relatively long time to perform, can be difficult to interpret, and is subject to movement of the fetus, it is used less frequently than ultrasonography as a diagnostic tool.
How Accurate Is an In-Utero Diagnosis of Hydrocephalus?
Prenatal ultrasound, performed by a radiologist or perinatologist skilled in obstetric ultrasound, is highly reliable and accurate. It will establish that there is an abnormal CSF collection, but it may not show the precise site of flow obstruction. The more important question is what caused the hydrocephalus and to what degree are there other malformations within the central nervous system. Amniocentesis (needle aspiration of intrauterine fluid) can of ten detect the presence of open neural tube defects, such as myelomeningocele, chromosome abnormalities and in utero infections, and may indicate the severity of the fetal condition. In general, early (first trimester) development of significant hydrocephalus can be a bad prognostic sign for infant mortality and developmental progress. In some cases, mild ventricular dilation identified by ultrasound has resolved itself by the third trimester.
What Happens After a Diagnosis Is Made or Suspected?
When enlarged ventricles are detected in a fetus, an evaluation is done to determine the cause of the intrauterine hydrocephalus. Because the cause of hydrocephalus—aqueductal stenosis, Dandy Walker, spina bifida, etc.—has a significant impact on associated conditions and long-term prognosis and treatment, the evaluation of cause is very important. Tests are also undertaken to look for other fetal abnormalities. Abnormalities in the fetal brain may indicate the presence of other system anomalies, prompting a search for other, subtler signs.
If hydrocephalus is detected or suspected, a more thorough high-level ultrasound examination should be performed to determine any associated CNS abnormalities (such as myelomeningocele or Dandy Walker), nonCNS abnormalities or other abnormalities of the heart or lungs. Amniocentesis also may be performed to assess the level of alpha-fetoprotein, which is elevated in cases of open neural tube defects; to search for abnormal chromosomes; and to determine fetal sex (males with hydrocephalus might have Xlinked aqueduct stenosis); as well as to rule out congenital infections. A scheduled series of ultrasounds over the term of pregnancy will be necessary to monitor ventricle size. The ultrasound study is a determination of the fetus at that particular time. There is usually no way to know whether ventricular size will increase or decrease on subsequent studies. It is important to have serial ultrasounds—although the frequency may depend upon how rapidly ventricular size is changing.
Once hydrocephalus has been confirmed, a number of medical specialists should become involved in care planning. If the family is given a diagnosis without immediate access to experienced specialists, it is likely that information and advice will come from well-meaning but unknowledgeable friends, relatives and even healthcare professionals. The pregnancy will now be considered “high risk,” and it is important for the expectant parents to have access to specialized, skilled, caring medical professionals. Additionally, if hydrocephalus is confirmed early in the pregnancy and the prognosis is very poor, counseling and support can be critical, as termination of the pregnancy may be an option for some parents.
One of the most important medical specialists to be consulted after the diagnosis of hydrocephalus is confirmed is a pediatric neurosurgeon with expertise in prenatal diagnosis. He/she is a highly skilled surgeon specializing in brain surgery in infants and children. Among those to be consulted are a perinatologist, a high-risk OBGYN, a geneticist and other prenatal specialists. A pediatric neuro surgeon’s active involvement on the medical team will insure that you receive the most accurate information regarding treatment options and the appropriate level of care and attention that your situation requires. Because a shunt will most likely be recommended for control of your child’s hydrocephalus after birth, establishing a relationship with a neurosurgeon as early as possible is very important. He/she can provide you with details about the shunting procedure as well as literature about hydrocephalus and appropriate follow-up medical care for your child. A skilled pediatric neurosurgeon most likely will be an integral member of your child’s medical team, following your child’s development for many years to come.
It is possible that the medical team will discuss delivering your baby by cesarean section or inducing delivery early, once it has been confirmed that the lungs are fully mature. Again, it is to your and your baby’s advantage to establish a plan of action with your extended medical team. Many families also find it helpful to visit the intensive care nursery (NICU) and the family room, and to learn about special services and resources available for high-risk deliveries.
How Is Prenatal Hydrocephalus Treated?
While some neurosurgeons have attempted in utero placement of a shunt, existing studies indicate that there are few benefits of doing so and, in fact, the potential complications outweigh the benefits. Although such procedures remain experimental and uncommon, further research on in utero and prenatal shunting is currently underway. It is generally felt that if ventricular size remains stable, the fetus should be followed to term. If progressive ventriculomegaly is demonstrated (that is, if the ventricles continue to enlarge), action may be taken sooner. Depending on gestational age and assessment of viability, several options are considered. For fetuses older than 35 weeks, a preterm cesarean section may be performed, and a shunt placed postnatally (after birth). For fetuses younger than 32 weeks, the risk of pulmonary (lung) immaturity must be weighed against the potential damage of progressive ventriculomegaly. As stated previously, it is important to develop a relation ship with your pediatric neurosurgeon during pregnancy so that he/she can provide you with details about shunting your baby after delivery.
Conclusion
There are many unknowns surrounding a prenatal diagnosis of hydrocephalus. This can be very frightening, distressing and sad for expectant parents, and extremely frustrating for the medical specialists who provide care. Although the outlook and success rate for infants diagnosed at or after birth is generally very high, there are limited studies avail able on the long-term prognosis of those with prenatal onset hydrocephalus. Much seems to depend on the extent of associated brain and systemic abnormalities, structural changes in the brain and the extent of the hydrocephalus. It is very difficult to accurately predict future function based on morphology or imaging. The more significant factor in the future development of children with prenatal onset hydrocephalus is the presence of continuing care and the absence of com plications such as infection or hemorrhage.
Because a prenatal diagnosis of hydrocephalus can be complex, it is essential that you learn as much as possible about your particular case so that you can make informed decisions. Establishing a strong relationship with the medical team, accepting that there may be unknowns about the severity of your child’s hydrocephalus and educating yourself and your family about hydrocephalus in general can help to alleviate your fears.
I would finally encourage you to consult your doctor at the beginning of the first trimester, so that you will remain aware of the fact that your child is safe and healthy, without any complicacies or in case there is an indication of developing any trouble, a doctor may be of a great help to avoid any unfair results.
The author is a teacher in Delhi Public School, Budgam and can be contacted at rihanbhat24@gmail.com