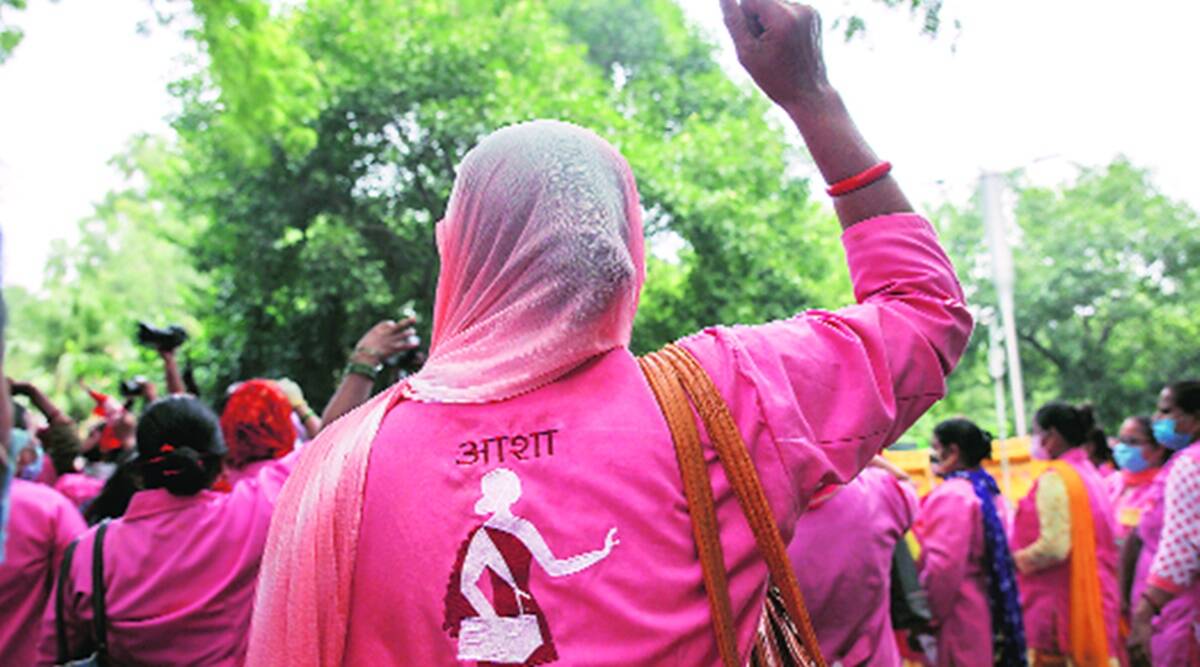By: Priyanka Saurabh
ASHA workers are volunteers from within the community who are trained to provide information and assist people in accessing the benefits of various health care schemes of the government. They act as a bridge connecting underserved communities with facilities such as primary health centers, sub-centers and district hospitals. The role of these community health volunteers was first established in 2005 under the National Rural Health Mission (NRHM).
ASHAs are primarily married, widowed, or divorced women between the ages of 25 and 45 within the community. They should have good communication and leadership skills; must be literate with formal education up to class 8 as per the program guidelines. The initiative aims at one ASHA for every 1,000 persons or habitation in hilly, tribal, or other sparsely populated areas.
There are about 10.4 lakh ASHA workers across the country, with the largest workforce in states with high populations – Uttar Pradesh (1.63 lacks), Bihar (89,437), and Madhya Pradesh (77,531). According to the latest National Health Mission data available from September 2019, Goa is the only state that does not have any such staff.
The World Health Organization has recognized the country’s 10.4 lacks ASHA (Accredited Social Health Activists) workers as ‘Global Health Leaders’ for their efforts to link the community with the government’s health programs. While this is commendable, women health volunteers continue to struggle for higher remuneration, regular jobs, and even health benefits.
While intermittent protests are taking place in several states, thousands of ASHA workers from across the country took to the streets in September last year to fight for their demands. ASHA (Accredited Social Health Activists) workers have received the Global Health Leaders Award-2022 against the backdrop of the 75th World Health Assembly. He was named “Guardian of the Year” by Time magazine in 2020.
ASHA workers go door-to-door in their designated areas to create awareness about basic nutrition, hygiene practices, and health services available. They primarily focus on ensuring that women receive antenatal check-ups, maintain nutrition during pregnancy, deliver in a health facility, and provide post-natal training on breastfeeding and complementary nutrition. Are. They also counsel women about contraception and sexually transmitted infections. ASHA workers have also been assigned the task of ensuring and motivating children to get vaccinated. In addition to mother and child care, ASHA workers also provide daily medicines to TB patients under Directly Observed Treatment under the National Program.
They are also tasked with checking for infections such as malaria during the season. They also provide basic medicines and treatments to the people under their jurisdiction such as oral rehydration solution, chloroquine for malaria, iron folic acid tablets to prevent anemia, and contraceptive pills. The health volunteers have also been tasked to inform their respective primary health centers about any birth or death in their designated areas. ASHA workers were an important part of the government’s pandemic response, with most states using networks to screen people in containment zones, test them, and move them to quarantine centers or help them to home quarantine. He went door-to-door to check the symptoms of Covid-19 among the people. Those who had a fever or cough, they had to be tested. They informed the officials and helped people reach the quarantine centers.
They visited homes with confirmed cases of COVID-19 and explained the quarantine process. He provided them with medicines and a pulse oximeter. All this was on top of his routine work. With the vaccination drive for Covid-19 starting in January last year, he has also been tasked with motivating people to get their shots and collecting data on how many are yet to be vaccinated. The problem faced by ASHA workers is that they are paid low and non-fixed wages and are not covered under minimum wages. There are more than 10.4 lakh ASHAs across India. In the last three years, ASHAs from at least 17 states have sought inclusion in social security schemes like fixed wages, higher incentives, and pensions. ASHAs are not recognized as workers and thus get less than Rs 18,000 per month. They are the cheapest healthcare provider in India.
Asha says she usually earns through antenatal care (Rs 300), institutional delivery (Rs 300), family planning (Rs 150), and vaccination rounds (Rs 100) as cases of other diseases are few. They are paid from NRHM funds for which they have to wait for a long time. The scheme has no dedicated budgetary allocation and funds are arranged on an ad-hoc basis from various government schemes such as the National Immunization Program under NRHM. Delay in reimbursement of incentives has hurt the self-esteem of ASHA workers and this has affected their service delivery. Instead of focusing only on community health care and related work, they are burdened with surveys and other non-related work.
In 2010, a parliamentary committee on women empowerment recommended a fixed salary for ASHAs. There should be a dedicated fund for ASHAs, which will ensure the timely payment of incentive amounts and boost the morale of the volunteers. Their skill upgradation should be an integral part of the plan. Volunteers should be encouraged to take short-term courses on Auxiliary Nurse Mid-Wife/General Nursing and Midwifery. This will not only help the volunteers get better incentives but also ensure that people living in remote areas have better health access. Currently, nursing schools in 11 states give preference to ASHAs for Auxiliary Nurse Mid-Wife and General Nursing courses.
In recent times, the Center has provided insurance coverage to ASHA workers and increased their honorarium. It should be institutionalized so that more and more community workers come forward and discharge their responsibilities effectively.
The writer is a Research Scholar in Political Science, Poet, freelance journalist and columnist.